Total shoulder replacement has helped many patients return to the activities they care about. That said, no surgical procedure comes without some degree of risk, and understanding the potential problems after shoulder replacement surgery can help you take an active role in your recovery and long-term outcome. In this post, we’ll explore the most common issues that may arise following a total shoulder replacement, with particular attention to glenoid loosening. We will also look at the modern technology designed to reduce these risks.
Key Takeaways
- Glenoid loosening is widely regarded as one of the most common reasons anatomic total shoulder replacements may require revision surgery over time.
- Advancements in shoulder implant technology are designed to reduce the likelihood of this complication.
- Choosing a surgeon who specializes in shoulder arthroplasty and utilizes advanced preoperative planning tools may help improve surgical planning accuracy and implant positioning.
A Brief Look at How Total Shoulder Replacement Works
Your shoulder is a ball-and-socket joint. The rounded top of your upper arm bone (the humeral head) fits against a shallow dish on your shoulder blade called the glenoid. Smooth cartilage covers both surfaces and allows the joint to glide without friction or pain.
Arthritis gradually wears that cartilage away. Pain increases, and motion decreases. During an anatomic total shoulder replacement, the surgeon removes the damaged surfaces and replaces them with artificial components. A metal implant takes the place of the humeral head, and a plastic component resurfaces the glenoid socket. The goal is to recreate the joint’s natural structure.
The results of this surgery tend to be very positive. However, like any major joint replacement, the procedure comes with possible complications.
Glenoid Loosening
Glenoid loosening occurs when the plastic socket component gradually separates from the underlying bone. It is widely regarded as one of the leading reasons an anatomic total shoulder replacement may require revision over time.
Why does this happen? Traditional glenoid designs rest on top of the bone surface. Every time you move your arm, forces push against the implant. Over months and years, the implant can develop a subtle tilting motion, often described as a “rocking horse” effect. That repeated rocking places concentrated stress on the edges, slowly breaking down the bond between the implant and bone.
How the Loosening Process Typically Unfolds
Glenoid loosening does not happen overnight. It tends to progress through stages, though the timeline varies from patient to patient.
In the earliest phase, tiny movements develop at the boundary between the implant and bone. These movements are microscopic, and you likely would not notice any symptoms. As this micromotion continues, the body may respond to implant wear particles with an inflammatory reaction that can contribute to gradual bone loss around the implant, a process known as osteolysis. Small cracks may form in the cement layer. Some patients begin to notice mild discomfort or a sense that their shoulder does not feel as stable as it once did.
When loosening reaches a more advanced stage, symptoms tend to become harder to ignore. Pain may return or worsen with activity. Range of motion can decrease. Some patients describe clicking, grinding, or a clunking sensation. In severe cases, the component may shift on X-ray imaging, and revision surgery could become necessary.
It is worth emphasizing that not everyone who receives a shoulder replacement experiences loosening. Several variables can influence whether glenoid loosening develops. Bone quality at the time of surgery matters. Patients with softer or less dense bone may struggle to achieve solid initial fixation. The positioning and alignment of the implant also play a role. Even small deviations in angle can change how forces distribute across the component. Activity level matters, too. Repeated heavy loads on the shoulder can accelerate wear over time.
How New Technology Aims to Solve This Problem
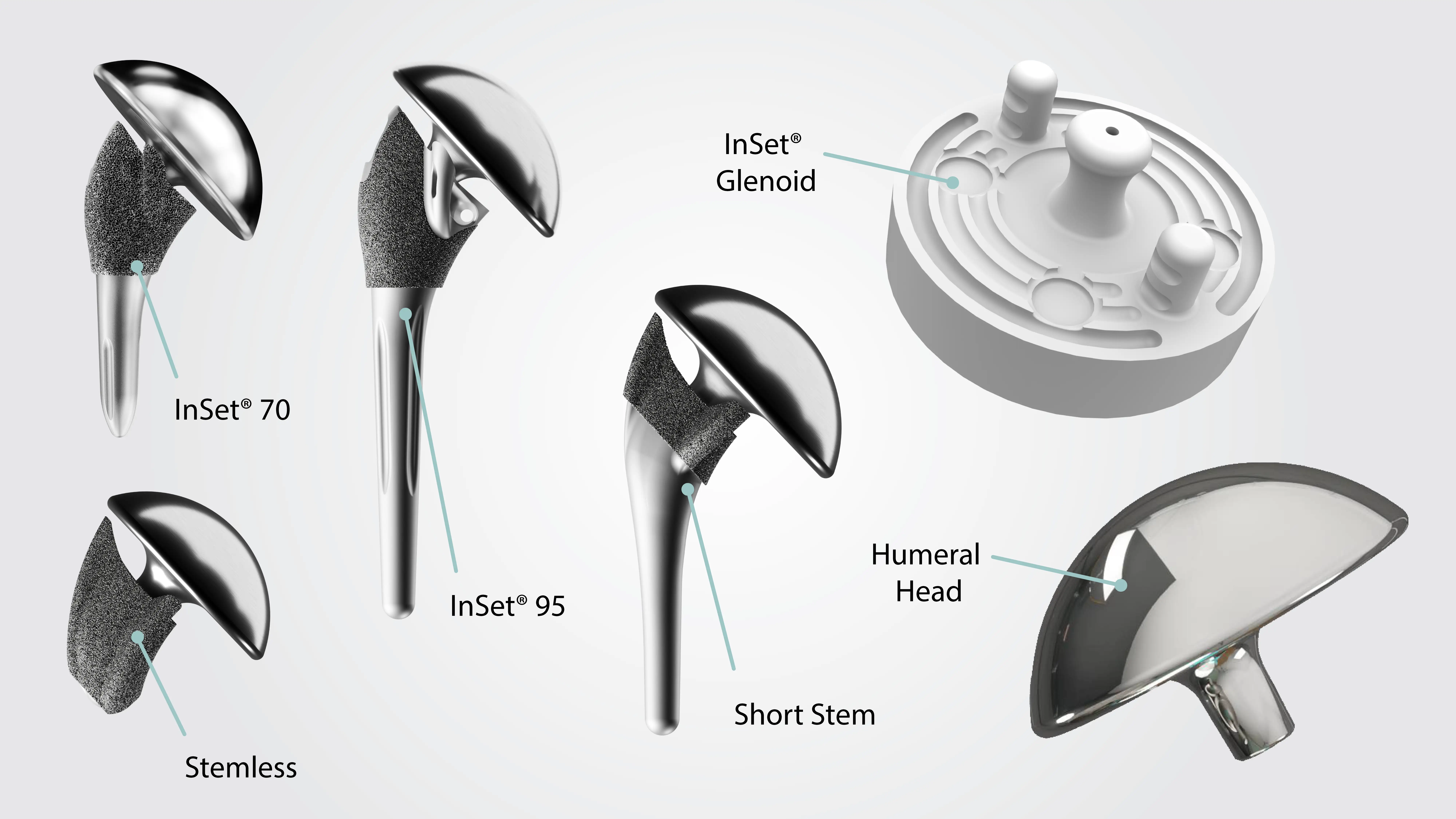
Given that glenoid loosening has been such a persistent challenge in shoulder arthroplasty, a great deal of engineering effort has gone into designing a better solution. The InSet® Shoulder System from Shoulder Innovations represents a meaningful step forward, and it is the system I use in my practice.
The fundamental difference lies in how the glenoid component interacts with the bone. Instead of sitting on top of the bone surface, the InSet® glenoid is placed within a pocket carved into the dense, sclerotic bone of the shoulder blade. Think of a manhole cover set flush into a street. Vehicles drive over it daily, yet it stays stable because it is recessed and surrounded by strong material. That concept inspired this design.
By seating the implant within a rim of strong bone, the InSet® design distributes forces more evenly across the component. Computer-based mechanical testing, known as Finite Element Analysis, has demonstrated up to an 87% reduction in modeled rocking horse stresses linked to loosening. The surrounding bone acts as a protective barrier, resisting the tilting motion that loosens traditional designs.
The Role of Pre-Operative Planning
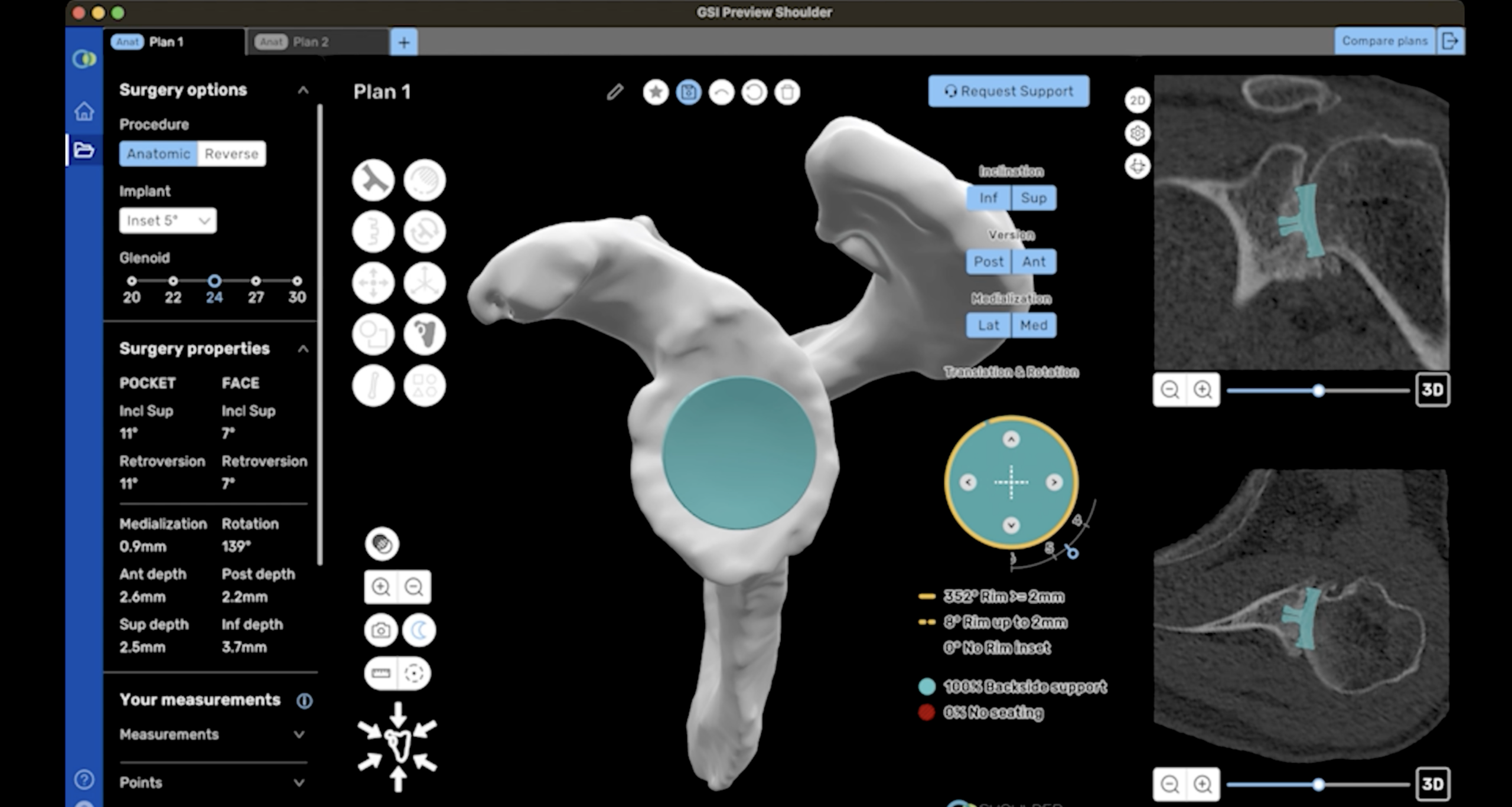
Implant design is only part of the equation. Where and how the component is positioned within your unique anatomy matters as well. That is why I also use ProVoyance®, an advanced software platform that allows me to plan the surgery in three dimensions before entering the operating room. Using detailed imaging, ProVoyance® helps me determine the optimal size, position, and angle for each component based on your specific bone structure. This patient-specific planning may reduce the risk of malpositioning, one of the contributing factors to loosening and other complications.
Other Potential Problems After Shoulder Replacement Surgery
While glenoid loosening gets much of the attention, it is not the only complication that can follow a total shoulder replacement. Being aware of other risks helps you and your team catch issues early.
Infection
Post-surgical infection is relatively uncommon, but it requires attention when it does occur. An infection may develop at the incision surface or deep within the joint. Deeper infections can sometimes require additional surgery to clean the area and, in some situations, temporarily remove the implant. Warning signs include increasing pain, redness, swelling, warmth near the surgical site, drainage from the wound, and fever.
Instability and Dislocation
After replacement, the ball component needs to stay seated within the socket. If it shifts, that is considered instability. Complete dislocation represents a more severe form of instability. Proper sizing and positioning of components during surgery help prevent this problem, as do healthy rotator cuff muscles and surrounding soft tissues. Patients with significant rotator cuff damage before surgery may face a higher risk. Symptoms may include a sense that the shoulder might give way or a clunking during movement.
Nerve Injury
Nerves that control movement and sensation run close to the surgical area. The axillary nerve, which powers the deltoid muscle, can be especially vulnerable. Nerve injuries after shoulder replacement may be temporary and resolve over time, although cases of persistent nerve dysfunction have been reported. Numbness, tingling, or weakness may occur but often resolve over weeks and months. Physical therapy can support recovery.
Rotator Cuff Complications
The rotator cuff is a group of tendons that stabilize and power your shoulder. A tear in these tendons after replacement can compromise function and potentially lead to instability. Some patients enter surgery with pre-existing damage that may progress over time. Protecting the rotator cuff through rehabilitation is an important part of the post-operative plan.
Persistent Stiffness
Some stiffness in the early weeks after surgery is completely expected. Your body is healing. However, stiffness that lingers or limits your daily activities may indicate a concern. Excessive scar tissue, insufficient rehabilitation, or suboptimal component positioning can contribute. Staying consistent with physical therapy is one of the most effective ways to combat this issue.
Practical Steps to Reduce Your Risk of Complications
While no one can guarantee a complication-free surgical experience, there are concrete steps you can take to tilt the odds in your favor. Here is what I encourage my patients to focus on.
Work with an Experienced Shoulder Specialist
Shoulder replacement is a technically demanding procedure, and carefully selecting an experienced shoulder specialist is an important step in the process. During your consultation, feel free to ask about your surgeon’s experience, annual case volume, and the technology they use.
Prepare Your Body Before Surgery
The healthier you are going into the operating room, the better your body may respond afterward. Managing chronic conditions like diabetes or high blood pressure ahead of time helps lay a stronger foundation. If you smoke, quitting at least several weeks before may reduce complications. Your surgeon may also adjust certain medications or recommend nutritional supplementation beforehand.
Commit to Your Rehabilitation Program
Physical therapy is often a component of successful recovery. Your therapist will guide you through exercises designed to restore motion, rebuild strength, and improve function. Early sessions typically focus on gentle, passive movements. As tissues heal, the program advances to active strengthening. Consistency matters.
Respect Your Shoulder’s New Limits
Modern implants are durable, but they are not indestructible. High-impact activities, contact sports, and repetitive heavy overhead lifting can place excessive stress on components. Most shoulder surgeons suggest avoiding these after replacement. Lower-impact pursuits like swimming, golf, and walking are generally encouraged. Talk with your surgeon about your specific goals.
Stay in Communication with Your Surgeon
Open dialogue with your surgical team is one of the simplest and most valuable things you can do. Do not wait for your next scheduled appointment if you experience increasing pain, sudden loss of motion, signs of infection, or a sense that your shoulder feels unstable. Catching problems after shoulder replacement surgery early may give your care team a better opportunity to intervene effectively.
Warning Signs That Deserve Prompt Attention
While some discomfort is normal during recovery, certain symptoms should prompt you to contact your surgeon’s office right away:
- Pain that worsens over time or does not respond to prescribed medication
- Fever, chills, or other signs suggesting infection
- Significant swelling, redness, or drainage at the incision site
- A sudden drop in your range of motion or strength
- A feeling that your shoulder may be slipping or shifting out of place
- Worsening numbness or weakness in your arm or hand
Your surgical team would much rather hear from you early than discover a problem that has progressed.
Summary
Total shoulder replacement has given many patients a path back to comfortable, active living after arthritis or injury made daily tasks painful. Like any major procedure, it carries some risks. Glenoid loosening stands out as the most common long-term threat to an anatomic shoulder replacement, though modern technology is making real progress. Your role matters, too. Preparing well, choosing a surgeon with deep shoulder arthroplasty experience, committing to rehabilitation, and maintaining open communication with your care team can all support a positive outcome.
Frequently Asked Questions
What exactly is glenoid loosening, and why does it matter?
Glenoid loosening refers to the gradual separation of the plastic socket component from the shoulder blade bone. It matters because it is considered the most common mechanical reason an anatomic total shoulder replacement may need revision. As the implant loosens, patients can experience returning pain and decreased range of motion.
Can glenoid loosening be prevented entirely?
No surgical technology can guarantee that loosening will never occur. However, advances in implant design have significantly reduced the risk. The InSet® glenoid component is engineered to sit within a pocket of strong bone, which has been shown to reduce associated mechanical stresses by up to 87% in computer modeling studies. Proper positioning and following post-operative activity guidelines may also help.
What activities should I avoid after a total shoulder replacement?
Most shoulder surgeons recommend steering clear of contact sports, heavy overhead lifting, and high-impact activities. Activities with a significant fall risk should also be approached with caution. Your surgeon can provide personalized guidance based on your specific circumstances.
Is some pain normal after shoulder replacement, or should I be worried?
Some post-operative discomfort is expected as your body heals. This should gradually improve over weeks and months. However, pain that worsens, returns after improvement, or comes with symptoms like fever or swelling may warrant evaluation. When in doubt, call and ask.



