Shoulder pain that builds gradually over months or years can be frustrating and, at times, confusing. If you have been told that you have a degenerative shoulder, this is likely referring to shoulder osteoarthritis, a condition in which the protective cartilage inside the joint slowly wears away over time. You may also hear it called degenerative joint disease. Whatever the name, the underlying issue is the same: the smooth cartilage that allows your shoulder to move freely breaks down, leading to pain, stiffness, and reduced function.
Degenerative shoulder conditions are a common reason patients seek orthopedic evaluation, particularly as they age. While osteoarthritis is the primary condition associated with this term, a degenerative shoulder can also involve rotator cuff deterioration and acromioclavicular joint arthritis.
Key Takeaways
- A degenerative shoulder most commonly refers to shoulder osteoarthritis, also known as degenerative joint disease, where the cartilage lining the joint gradually wears down.
- Symptoms typically include persistent pain, stiffness, grinding or crunching sensations, and a progressive loss of range of motion.
- Treatment generally begins with conservative options like physical therapy, medications, and injections, and may progress to surgical intervention when necessary.
What Is a Degenerative Shoulder?
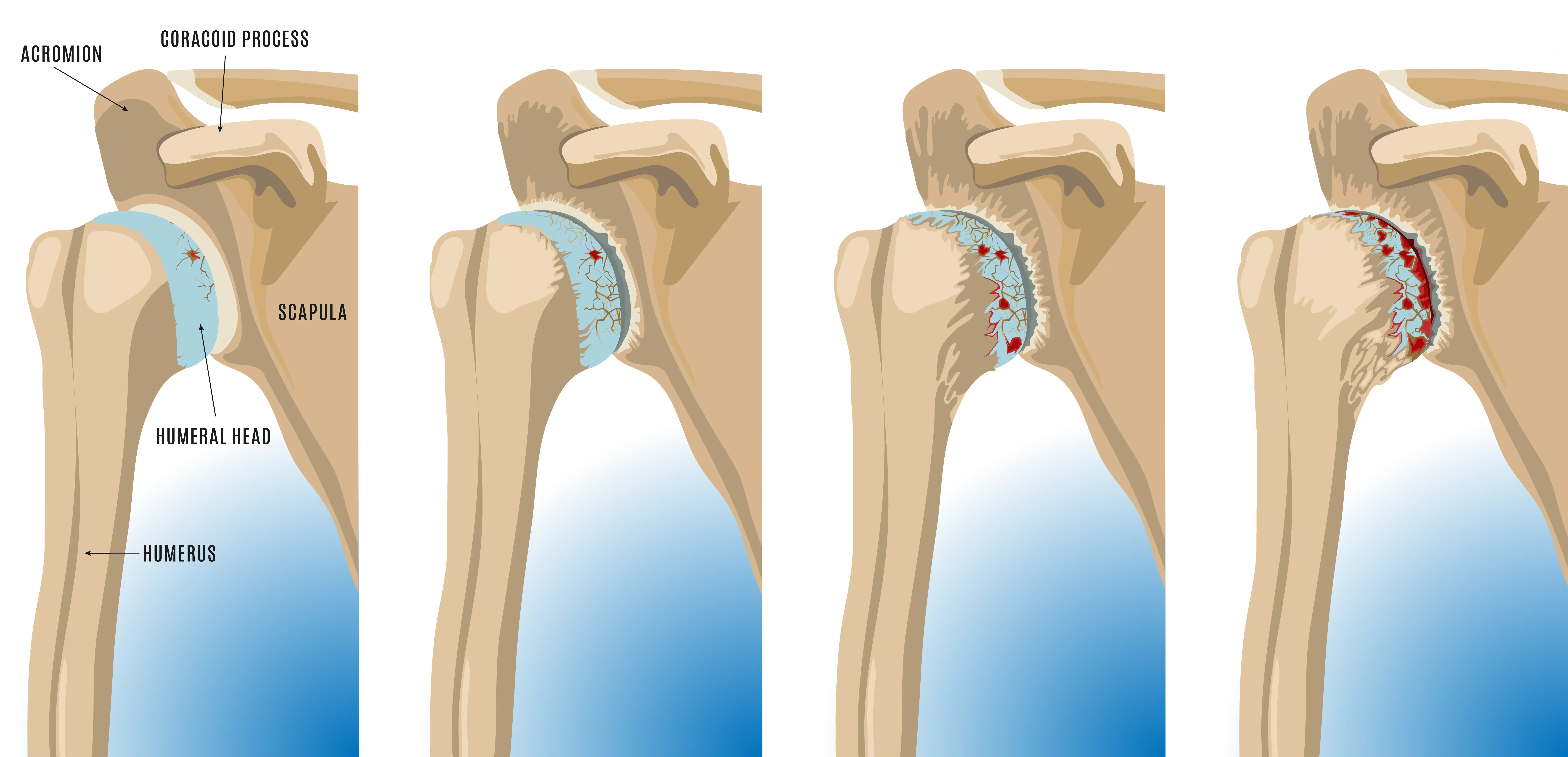
Degenerative shoulder primarily refers to osteoarthritis of the shoulder joint. Osteoarthritis is a common form of arthritis, and it develops when the articular cartilage, the smooth, protective tissue covering the ends of the bones, gradually deteriorates. In a healthy shoulder, this cartilage allows the ball of the upper arm bone (humeral head) to glide smoothly within the socket of the shoulder blade (glenoid). When that cartilage wears thin, the bones begin to rub against each other, creating friction, inflammation, and pain.
This process tends to happen slowly. In its early stages, the cartilage softens and develops surface cracks. Over time, it may begin to flake and wear away entirely. In advanced cases, the joint becomes bone-on-bone, meaning there is little to no cartilage left to cushion movement. The body may attempt to stabilize the joint by forming bone spurs (osteophytes), which can further limit motion and cause discomfort.
Shoulder osteoarthritis most often affects the glenohumeral joint, the main ball-and-socket joint of the shoulder. However, the acromioclavicular (AC) joint at the top of the shoulder can also develop degenerative changes. Some patients experience arthritis in both joints simultaneously.
What Causes Shoulder Osteoarthritis?
Shoulder osteoarthritis can be classified as either primary or secondary. Primary osteoarthritis has no single identifiable cause. It tends to develop with age as the cartilage naturally loses its resilience and water content. Genetics may also play a role, and individuals with a family history of osteoarthritis may have a higher likelihood of developing the condition.
Secondary osteoarthritis develops as a result of a known factor. A previous shoulder injury, such as a fracture or dislocation, can damage the cartilage directly or alter the joint’s mechanics in a way that accelerates wear over time. Repetitive overhead activities, whether from sports like swimming and tennis or from occupational demands like construction or painting, can place cumulative stress on the joint.
Related Conditions That Can Accompany Shoulder Degeneration
While osteoarthritis is the core condition behind a degenerative shoulder, it may not exist in isolation. Several related problems can develop alongside it or contribute to the shoulder’s overall decline.
Degenerative Rotator Cuff Tears
The rotator cuff is a group of four tendons that stabilize the shoulder and control arm movement. Over time, these tendons can weaken, fray, and eventually tear as part of the aging process. Reduced blood supply to the tendon tissue, repetitive motion, and normal wear all contribute. Degenerative rotator cuff tears are common in patients over 50 and may occur with or without significant symptoms.
When a large rotator cuff tear goes untreated for an extended period, the humeral head can migrate upward within the joint, accelerating cartilage wear. This combination of a massive rotator cuff tear and advanced arthritis is known as rotator cuff tear arthropathy.
Acromioclavicular (AC) Joint Arthritis
The AC joint sits at the top of the shoulder where the collarbone meets the shoulder blade. This small joint is particularly vulnerable to degenerative changes, especially in people who perform repetitive overhead work or heavy lifting. Prior AC joint injuries, such as separations, can also predispose it to arthritis.
AC joint arthritis often produces localized pain at the top of the shoulder that worsens when reaching across the body or pressing overhead. While it affects a different part of the shoulder than glenohumeral osteoarthritis, both conditions can be present at the same time and may need to be addressed together.
Symptoms of a Degenerative Shoulder
The symptoms of shoulder osteoarthritis tend to develop gradually and worsen over time. Early on, you may notice a dull ache deep within the shoulder that flares up during or after activity. As the cartilage continues to break down, the pain often becomes more persistent and may begin to interfere with sleep.
Stiffness is another common symptom. Patients frequently report difficulty with overhead reaching, putting on a coat, or fastening items behind the back. As the cartilage wears away, many patients also notice grinding, clicking, or crunching sensations during shoulder movement. This is called crepitus, and it results from the roughened bone surfaces rubbing against each other.
Weakness may develop as well, usually because patients instinctively limit their use of the painful shoulder. Over time, this reduced activity can lead to muscle atrophy and further functional decline. Some patients also experience swelling or tenderness around the joint, particularly during flare-ups.
Many people adapt their habits without realizing it, avoiding movements that trigger pain. If you have noticed that your shoulder has been gradually getting stiffer, more painful, or harder to use over the past several weeks or months, those may be signs of degenerative changes worth having evaluated.
How Is a Degenerative Shoulder Diagnosed?
Diagnosing shoulder osteoarthritis typically begins with a thorough clinical evaluation. An experienced shoulder specialist will ask about the nature and duration of your symptoms, any previous injuries, your activity level, and how the pain affects your daily life. During the physical examination, they may assess your shoulder’s range of motion, strength, and areas of tenderness. Specific clinical tests can help determine which structures are involved.
X-rays are usually the first imaging study ordered. They may reveal signs of osteoarthritis, including narrowing of the joint space, the presence of bone spurs, and changes in the shape or alignment of the bones. In some cases, an MRI may be recommended to evaluate the soft tissues, particularly the rotator cuff tendons, to determine whether additional problems are present alongside the arthritis. A CT scan may be used when a more detailed bone assessment is needed, especially for surgical planning.
Non-Surgical Treatment Options
Treatment for a degenerative shoulder generally starts with conservative measures. Many patients achieve meaningful relief without surgery, especially when the condition is caught relatively early.
Physical therapy may be a component of the treatment plan. A structured rehabilitation program can help maintain and improve range of motion, strengthen the muscles that support the shoulder, and reduce pain. Your therapist can tailor exercises to your specific condition, beginning with gentle mobility work before gradually introducing resistance training.
Over-the-counter anti-inflammatory medications may be recommended to help manage pain and reduce inflammation. Corticosteroid injections may provide targeted, short-term relief within the joint and are often helpful during flare-ups, though they are generally not considered a long-term solution. Platelet-rich plasma (PRP) therapy, which uses a concentration of the patient’s own blood platelets to promote healing, may be an option for some patients with mild arthritis.
Adjusting daily habits, avoiding movements that aggravate the shoulder, and incorporating rest periods can help manage symptoms and may slow further deterioration. Ergonomic adjustments at work and proper body mechanics during physical activity can also reduce stress on the joint.
Surgical Treatment Options
When conservative treatments no longer provide adequate relief, surgical intervention may be recommended. The right procedure depends on the severity of the arthritis, the condition of the rotator cuff, and the patient’s overall health and goals.
Arthroscopic Surgery
Shoulder arthroscopy is a minimally invasive procedure that uses a small camera and specialized instruments inserted through tiny incisions. It may be used in selected patients to remove loose bodies, clean out inflamed tissue, or address bone spurs. While arthroscopy can be helpful for milder forms of arthritis, it generally does not stop the progression.
Shoulder Replacement Surgery
For patients with severe shoulder osteoarthritis, shoulder replacement surgery (arthroplasty) may be considered. The procedure may provide substantial pain relief and improved function for appropriately selected patients.
There are two main types of shoulder replacement surgery. A total (anatomic) shoulder replacement replaces both the ball and the socket and is generally best suited for patients whose rotator cuff remains intact. A reverse shoulder replacement switches the position of the ball and socket, allowing the deltoid muscle to power the arm instead of the rotator cuff. This approach has become increasingly common and is often the preferred option for patients who have both arthritis and significant rotator cuff damage, such as those with rotator cuff tear arthropathy.
Summary
A degenerative shoulder is most commonly a reference to shoulder osteoarthritis, a condition in which the cartilage protecting the joint gradually wears away, leading to pain, stiffness, and reduced mobility. While osteoarthritis is the primary condition behind this term, related problems like degenerative rotator cuff tears and AC joint arthritis may develop alongside it, compounding the impact on shoulder function.
A wide range of treatment options exists. Conservative approaches such as physical therapy, medications, injections, and activity modifications may be effective for many patients. When those measures are no longer enough, surgical options including shoulder replacement may be recommended.
Frequently Asked Questions
What does it mean when a doctor says I have a degenerative shoulder?
In most cases, a degenerative shoulder refers to shoulder osteoarthritis, also called degenerative joint disease. This means the cartilage inside your shoulder joint has been gradually wearing down, causing pain, stiffness, and reduced motion. Your doctor may also evaluate whether related problems, such as rotator cuff damage or AC joint arthritis, are contributing to your symptoms.
Can a degenerative shoulder get better without surgery?
Yes, some patients manage degenerative shoulder conditions effectively without surgery. Physical therapy, anti-inflammatory medications, injections, and activity modifications can help reduce pain and improve function. That said, osteoarthritis can be progressive over time, and some patients may eventually consider surgical intervention if conservative treatments no longer provide adequate relief.
When should I see a specialist about my shoulder pain?
Consider scheduling an appointment if your shoulder pain has persisted for more than a few weeks, interferes with daily activities or sleep, or is accompanied by stiffness, weakness, or grinding sensations. Early evaluation can help identify degenerative changes before they progress significantly.



