When the shoulder joint suffers from severe damage, pain, and loss of function, it can become debilitating. For patients facing this challenge, shoulder joint replacement, also known as shoulder arthroplasty, may offer a possible path to pain relief and restored mobility. In this post, we’ll explore the conditions that lead to this procedure, the differences between the two main types (total and reverse), and what patients may expect on their journey to recovery.
Key Takeaways
- Total shoulder replacement, or anatomic arthroplasty, may be recommended when the rotator cuff tendons are healthy and the primary issue is severe arthritis.
- Reverse shoulder replacement may be used for patients with both severe arthritis and an irreparable rotator cuff tear (cuff tear arthropathy), reversing the ball-and-socket configuration to allow the deltoid muscle to power the arm.
- Recovery frequently involves a structured physical therapy program and a commitment to protecting the new joint, with the goal of returning to a more active and pain-free lifestyle.
When to Consider Shoulder Joint Replacement
Patients often live with increasing discomfort for years before exploring options for relief. Recognizing possible symptoms that may suggest a shoulder joint replacement can be the first step toward finding relief.
Persistent and Severe Pain
Shoulder pain is the most common reason patients seek treatment, often described as a deep, aching sensation within the joint. For many, the pain becomes severe enough to interrupt sleep and may continue even when the arm is completely at rest. Simple movements can trigger sharp or shooting pain, making daily activities difficult. There can often be a sensation of clicking, catching, or popping in the shoulder as the rough bony surfaces rub against each other. Over-the-counter pain relievers and anti-inflammatory medications may offer temporary improvement, but they frequently fail to provide lasting relief.
Loss of Motion and Stiffness
As the joint surfaces wear down or the surrounding tissues become damaged, the shoulder’s natural mobility begins to decline. This loss of motion is one of the most noticeable signs of advanced joint disease. Patients often struggle to lift their arm away from their side or raise it overhead, and everyday tasks like reaching behind the back to tuck in a shirt may become nearly impossible.
Functional Limitations
The shoulder’s primary job is to position the hand in space, which makes it essential for most daily movements. When the joint becomes compromised, even basic tasks like washing hair, getting dressed, or reaching into a cupboard can become difficult. The loss of function often affects a person’s independence and overall quality of life.
When these symptoms stop responding to conservative treatments, a surgeon may recommend shoulder joint replacement as a potential way to restore comfort, mobility, and function.
Conditions Treated by Shoulder Joint Replacement
The most common conditions treated by this procedure involve the breakdown of the joint’s smooth cartilage.
Osteoarthritis (Wear-and-Tear Arthritis)
This is the most frequent reason for a total shoulder replacement. Osteoarthritis involves the progressive breakdown of the articular cartilage that covers the ends of the bones. Due to wear-and-tear over time, the cartilage thins and frays, and may cause the bones to rub against each other. This friction can lead to pain, stiffness, and the formation of bone spurs.
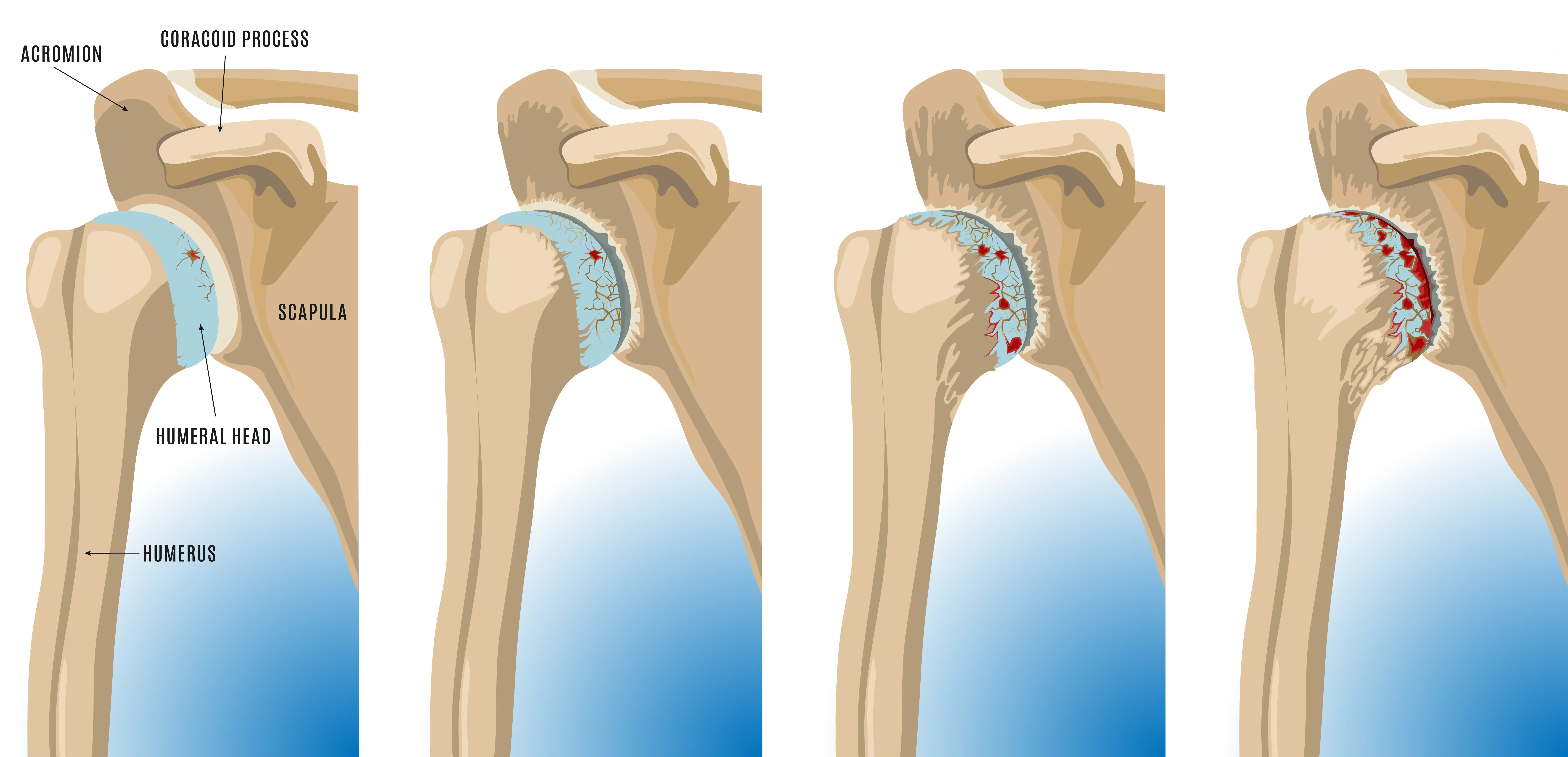
Rheumatoid Arthritis
Rheumatoid arthritis is an autoimmune disease. It causes the body’s immune system to attack the lining of the joint capsule. Unlike osteoarthritis, it often affects both shoulders symmetrically.
Post-Traumatic Arthritis
This type of arthritis develops after a significant shoulder injury. Fractures or severe dislocations can damage the joint surfaces or alter the shoulder’s mechanics. The initial injury may accelerate the wear-and-tear process.
Cuff Tear Arthropathy
This is a form of arthritis that occurs when a large, long-standing rotator cuff tear is present alongside advanced arthritis. In cuff tear arthropathy, the torn rotator cuff can no longer stabilize the humeral head (the ball). The humeral head moves upward and rubs against the acromion (part of the shoulder blade). This abnormal contact may cause significant pain.
Severe Fractures
In some cases, a severe fracture of the upper arm bone (humerus) may shatter the bone into many pieces. If the blood supply to the bone fragments is compromised, a replacement may be a recommended option.
Total Shoulder Replacement
Total shoulder replacement, also known as anatomic total shoulder arthroplasty, is the traditional form of shoulder joint replacement. The goal is to replicate the shoulder’s natural ball-and-socket anatomy to provide pain relief and improve function.
Total shoulder replacement is generally a preferred option for patients whose primary problem is severe arthritis. These patients must have a healthy, functional rotator cuff, as these muscles are essential for controlling the movement of the new joint.

Reverse Shoulder Replacement
Reverse shoulder replacement is an advancement in orthopedic surgery. It was developed specifically to address the complex problem of cuff tear arthropathy. It may also be used to address complex shoulder fractures. Unlike the total shoulder replacement, this replacement reverses the natural anatomy of the joint.
The name “reverse” describes the implant’s unique configuration. The surgeon switches the position of the ball and socket components. A metal ball is fixed to the shoulder blade, and a plastic socket is placed on top of the humerus. This design allows the large deltoid muscle to take over the function of the damaged rotator cuff.

The Surgical Process and Recovery
Pre-Operative Planning
Your surgeon will likely conduct a thorough evaluation before recommending surgery. This could include a complete medical history, imaging tests, and a discussion of the risks, benefits, and expected recovery timeline.
The Procedure
Both total and reverse shoulder replacement procedures are usually performed under general anesthesia. The surgery typically takes a few hours. The general steps are as follows:
- The surgeon makes an incision over the shoulder.
- They carefully move the muscles aside to access the joint.
- The damaged bone and cartilage are removed.
- The new metal and plastic components are implanted and secured.
- The surgeon closes the incision, and the patient is moved to the recovery room.
Post-Operative Recovery and Rehabilitation
Recovery is a gradual process that requires patience and commitment. The first few weeks focus on protecting the surgical repair. The arm is often immobilized in a sling for 1-2 weeks, with the exact timeline determined by the surgeon. Pain management is a priority in the immediate post-operative period. While there is pain from surgery, for patients with bad arthritis before surgery, their pain is often much better almost immediately following the procedure.
The Role of Physical Therapy
Physical therapy is often an important component of a successful recovery. The goal is to help the patient regain strength and range of motion. Initially, physical therapy may focus on passive range of motion, where the therapist moves the arm to prevent stiffness. The next phase may introduce active range of motion, where the patient begins to move the arm independently. The final phase generally concentrates on strengthening the muscles around the new joint.
Summary
Whether a patient requires a total or a reverse procedure, the goal remains the same: to alleviate pain and restore functional movement. An experienced shoulder surgeon will work closely with each patient to tailor a treatment plan that aligns with their personal goals and lifestyle. If chronic shoulder pain is limiting your life, consulting with a specialist may be the first step toward regaining mobility and returning to activities you love.
Frequently Asked Questions
What is the difference between a total shoulder replacement and a reverse shoulder replacement?
The main difference lies in the patient’s underlying condition and the implant’s design. A total shoulder replacement may be recommended for patients with a healthy rotator cuff. It primarily addresses shoulder arthritis by mimicking the natural anatomy (ball on the arm bone, socket on the shoulder blade). A reverse shoulder replacement may be used for patients with a damaged rotator cuff (cuff tear arthropathy), as it reverses the anatomy (ball on the shoulder blade, socket on the arm bone). This reversal allows the deltoid muscle to power the arm, compensating for the rotator cuff.
Will I be able to play sports after my shoulder joint replacement?
Many patients return to low-impact activities and sports. These may include swimming, golf, and tennis. High-impact sports or activities involving heavy lifting, repetitive overhead motion, or a high risk of falling may be generally discouraged. Your surgeon will provide specific recommendations based on your procedure, recovery, and the type of implant used.
How long is the recovery period?
The recovery period varies significantly among patients. The initial recovery, involving the use of a sling, typically lasts around four to six weeks. Significant functional improvement often occurs between three and six months after surgery. Full recovery, including maximum strength and range of motion, can take up to a year or longer.



