One wrong move, a hard fall, or a collision on the field, and suddenly something feels seriously, undeniably wrong. If you’ve ever found yourself asking how to tell if your shoulder is dislocated, you’re in good company. Distinguishing a dislocated shoulder from other injuries can be difficult without a proper medical evaluation. However, there are several signs that may point in that direction, and knowing what to watch for, and what to do about it, can make a difference in how quickly you get the right care.
Key Takeaways
- A dislocated shoulder happens when the ball of the upper arm bone slips partially or fully out of the shoulder socket.
- Common signs may include sudden severe pain, visible deformity, swelling, and difficulty moving the arm.
- Shoulder dislocations are most often caused by falls, sports injuries, or significant trauma to the joint.
- Treatment may include manual reduction, rest, immobilization, physical therapy, and in some cases, surgery.
What Is a Shoulder Dislocation?
Your shoulder is a ball-and-socket joint. The rounded top of your upper arm bone, called the humeral head, sits inside a cup-shaped socket on your shoulder blade, known as the glenoid. When a dislocation occurs, that ball gets pushed out of the socket, either partially or completely. Because the socket is relatively shallow compared to, say, the hip joint, the shoulder is more vulnerable to displacement.
A partial dislocation, sometimes called a subluxation, means the ball slips out of position but may shift back on its own. A full dislocation means the ball has come completely free from the socket and won’t return without medical intervention.
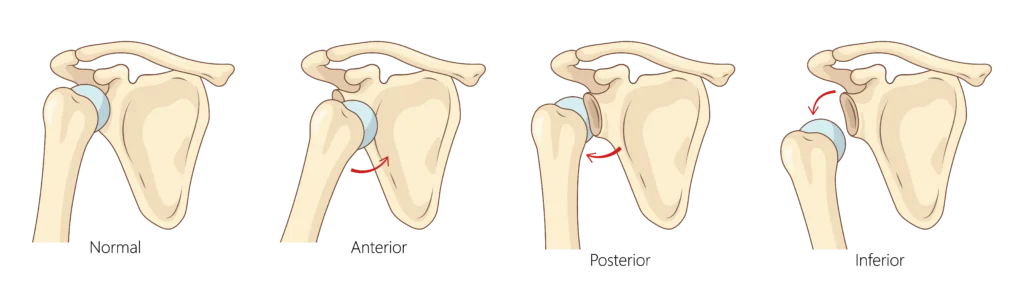
Signs That Your Shoulder May Be Dislocated
How can you tell if your shoulder is dislocated? The experience can vary depending on the severity of the injury and the direction of the displacement, but several symptoms tend to be present.
Sudden, Severe Pain
The pain associated with a dislocated shoulder is typically immediate and intense. It tends to be centered around the shoulder joint and may radiate down into the arm or toward the neck. Moving the arm, even slightly, usually makes the pain significantly worse. Most people find the discomfort difficult to ignore.
Visible Deformity
This is one of the more telling signs. A dislocated shoulder often looks visibly different from a healthy one. The shoulder may appear squared off or flattened where it’s normally rounded. You might notice an unusual bump, bulge, or hollow that wasn’t there before. Comparing both shoulders can sometimes help. If one looks noticeably asymmetrical, that’s worth paying attention to.
Swelling and Bruising
Swelling around the shoulder joint tends to develop fairly quickly following a dislocation. Bruising may take several hours or even a day or two to fully appear. The presence of both swelling and bruising alongside pain and deformity may suggest an injury.
Inability to Move the Arm Normally
One of the clearest signals that something is seriously wrong is when you try to lift, rotate, or move your arm and simply can’t. Most people with a dislocated shoulder find normal arm movement impossible or so painful that they avoid attempting it altogether.
Numbness, Tingling, or Weakness
The nerves and blood vessels that travel through the shoulder region can be affected when the joint is displaced. You may feel numbness or a tingling, pins-and-needles sensation running into your arm, hand, or fingers. Weakness in the arm is also possible. These symptoms don’t occur in every case, but they may signal nerve involvement.
Muscle Spasms
Some people experience muscle spasms around the shoulder after a dislocation. The surrounding muscles may contract involuntarily, essentially trying to stabilize the joint on their own, which can intensify the overall pain.
What Causes a Shoulder Dislocation?
Shoulder dislocations generally happen because of a specific incident or event. The most common causes include falls, sports-related injuries, and trauma. Falling on an outstretched arm or landing directly on the shoulder can apply enough force to push the joint out of alignment. Contact sports like football, hockey, and wrestling carry a notably higher risk, as do activities that require frequent overhead motion, such as swimming or volleyball. Car accidents and other high-impact events can also result in dislocation if there’s enough force directed at the shoulder.
Once you’ve had a shoulder dislocation, your risk of experiencing another one may increase. The ligaments and other soft tissue structures that help hold the joint stable can be stretched or torn during the original injury. That damage can make the shoulder less reliable over time.
What to Do If You Think Your Shoulder Is Dislocated
If you suspect you have a dislocated shoulder, the most important thing to do is get medical attention as soon as possible. In the meantime, there are a few key things to keep in mind.
First, do not attempt to relocate the shoulder yourself. It may seem tempting, but forcing the joint back into place without medical training and the appropriate setting can cause serious additional harm, including nerve and blood vessel damage or a fracture.
Try to immobilize the arm in whatever position feels most comfortable. A sling works well, but even cradling the arm gently against your body helps limit movement and can reduce pain while you make your way to care. If ice is available, applying it (wrapped in a cloth, not directly on skin) to the shoulder may help manage swelling in the short term.
Prompt treatment generally supports better outcomes. Waiting too long can allow swelling to worsen, complicate the reduction process, and increase the likelihood of additional injury to the surrounding structures.
How Doctors Diagnose a Shoulder Dislocation
When you arrive at a medical facility, they will typically begin with a physical examination. They’ll assess the shape of the joint, your range of motion, your pain level, and the circumstances surrounding the injury. A thorough history of how the injury happened often gives important clues.
Imaging is usually needed to confirm a dislocation and check for any associated fractures. An X-ray is typically the first step. It can show the exact position of the displaced joint and reveal whether any bones have been broken in the process, something that affects how treatment proceeds. If soft tissue damage is suspected, an MRI may be ordered afterward to evaluate the labrum, ligaments, and surrounding structures in more detail.
Treatment Options
Once a dislocation is confirmed, the immediate goal is to guide the joint back into its proper position. This procedure is called a closed reduction, and it must be performed by a trained medical professional. Using carefully controlled movements, the ball can be maneuvered back into the socket. Many patients notice meaningful pain relief shortly afterward.
Following the reduction, the broader treatment plan may include several components:
- Immobilization: A sling or brace is commonly used for a period of time to allow the joint and surrounding tissues to begin healing.
- Medication: Over-the-counter or prescription anti-inflammatory medications and pain relievers may be recommended to help manage discomfort in the initial recovery period.
- Physical therapy: Rehabilitation is a key part of recovery. A physical therapist can guide you through targeted exercises designed to restore strength, stability, and range of motion progressively and safely.
- Surgery: In cases where the dislocation has caused significant structural damage, such as tears to the labrum or ligaments, or in patients who experience recurrent dislocations, surgical intervention may be recommended.
Recovery: What to Expect
Recovery from a shoulder dislocation looks different for everyone. The severity of the injury, your age, your overall health, and whether additional damage occurred all play a role in how long healing takes. For a first-time, uncomplicated dislocation, many people begin feeling meaningfully better within a few weeks. That said, maximal recovery can take considerably longer.
Following a prescribed physical therapy program may help improve strength and stability over time. Skipping exercises or returning to activity too soon can slow the healing process and raise the risk of re-injury. Patience matters here, even when progress feels slow.
If surgery is part of your treatment plan, recovery timelines will naturally extend further. Whether your goal is getting back on the field, returning to work, or simply being able to reach a cabinet without pain, the approach is tailored to what matters most to you.
When to See a Shoulder Specialist
If you’ve already been evaluated for a shoulder dislocation but you’re still dealing with ongoing shoulder instability, persistent discomfort, or repeated episodes of the joint slipping out of place, it may be time to connect with an experienced shoulder specialist. These experiences may indicate that the supporting structures of the shoulder sustained damage during the original injury and have not healed adequately on their own.
Summary
The signs most commonly associated with a dislocation include sudden severe pain, visible deformity, swelling, inability to move the arm normally, and possible numbness or tingling. If you think your shoulder might be dislocated, avoid any attempt to self-correct it, immobilize the arm as best you can, and get to a medical facility.
Frequently Asked Questions
Can a dislocated shoulder heal on its own?
A dislocated shoulder often requires medical treatment to return to its proper position. Waiting to see whether the pain improves on its own is generally not recommended, as the joint is unlikely to reposition itself and additional damage may occur in the meantime. Seeking evaluation promptly gives you the best chance at a smooth recovery.
How painful is a shoulder dislocation?
Most people describe the pain as immediate and severe. The level of discomfort may vary depending on the person and the extent of the injury, but shoulder dislocations are widely considered to be quite painful.
Is surgery always required for a dislocated shoulder?
Surgery is not necessary in every case. Many patients recover well with non-surgical approaches, including reduction, immobilization, and physical therapy. Surgical intervention tends to be considered when structural damage is present, or when a patient continues to experience recurrent dislocations despite conservative treatment.



