Persistent discomfort can stem from shoulder arthritis, a condition characterized by the inflammation and degeneration of the joint’s cartilage. In this post, we’ll take a close look at the symptoms of shoulder arthritis, along with diagnostic approaches and treatment options.
Key Takeaways
- Key symptoms include persistent pain (often worsening with activity and at night), stiffness, decreased range of motion, grinding or popping sensations (crepitus), and sometimes weakness or swelling.
- Factors such as age, genetics, previous injuries, inflammatory conditions, and overuse can contribute to the development and progression of shoulder arthritis.
- Accurate diagnosis relies on a thorough medical history, physical examination, and imaging studies.
- Management ranges from conservative non-surgical methods (medications, physical therapy, activity modification, injections) to advanced surgical interventions.
Types of Shoulder Arthritis
Understanding the specific type of shoulder arthritis is important for effective diagnosis and tailored treatment, and it can also impact the symptoms an individual may experience.
Osteoarthritis (Degenerative Joint Disease)
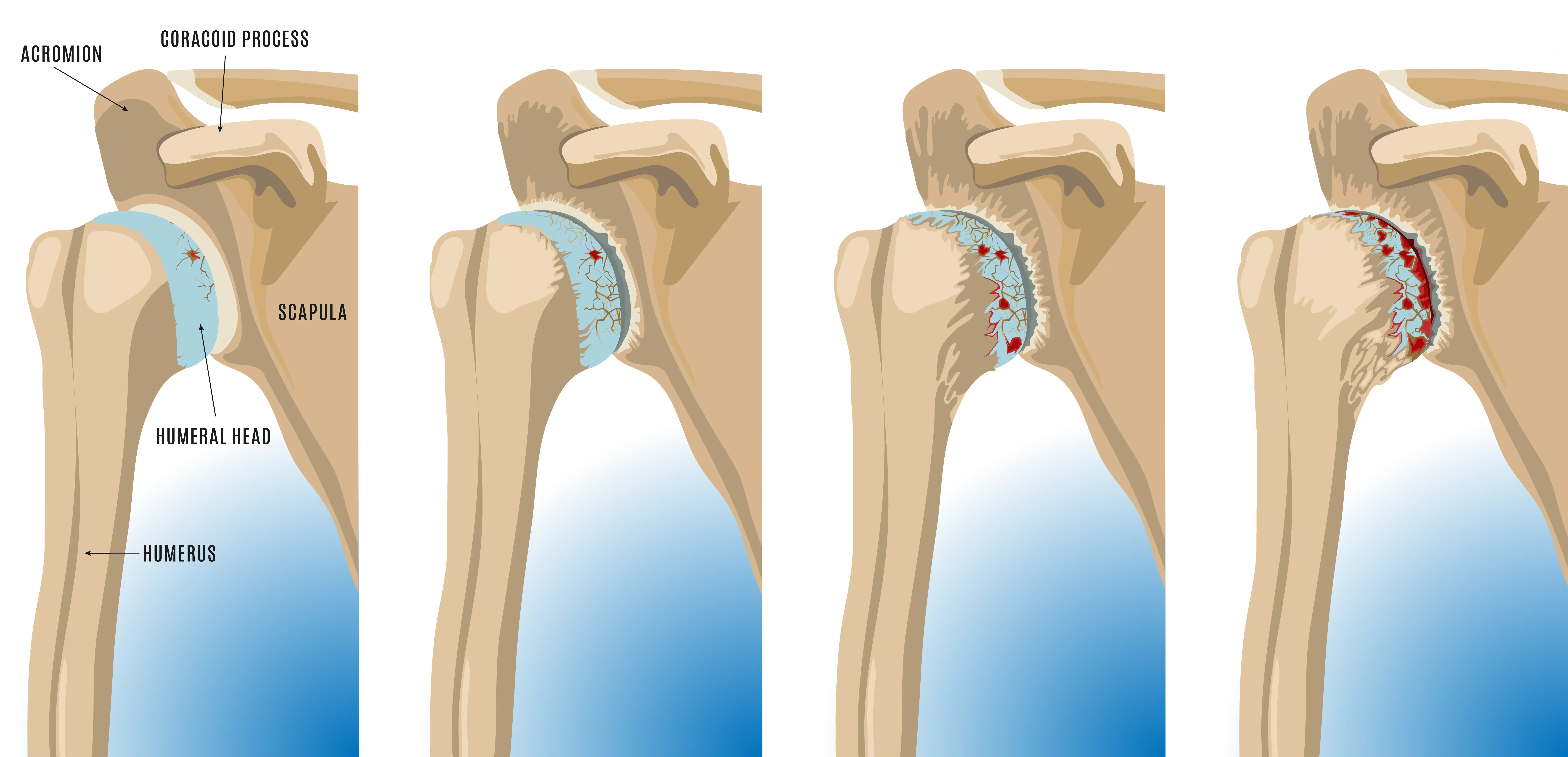
Osteoarthritis (OA), also known as degenerative joint disease or wear-and-tear arthritis, is the most common form of shoulder arthritis. It typically develops gradually over time as the smooth articular cartilage that covers the ends of the bones in the shoulder joint deteriorates. As the cartilage erodes, the protective space between the bones narrows. As the cartilage wears worsens it may eventually lead to the bones rubbing against each other (bone-on-bone arthritis).
Rheumatoid Arthritis (Inflammatory Arthritis)
Rheumatoid arthritis (RA) is a chronic autoimmune disease where the body’s immune system mistakenly attacks its own tissues, including the lining of the joints (synovium). This attack leads to inflammation, pain, swelling, and eventually, erosion of cartilage and bone. Unlike osteoarthritis, which often affects one joint or side of the body, RA typically affects multiple joints symmetrically.
Post-traumatic Arthritis
Post-traumatic arthritis can develop after a physical injury to the shoulder, such as a fracture or a dislocation. The injury can damage the articular cartilage directly or alter the mechanics of the joint, leading to accelerated wear and tear that mimics osteoarthritis.
Rotator Cuff Tear Arthropathy
Rotator cuff tear arthropathyis a form of shoulder arthritis that occurs in conjunction with a large, long-standing rotator cuff tear. The rotator cuff muscles are important for stabilizing and moving the shoulder joint. When these tendons are extensively torn and left unrepaired, the humeral head (the ball of the shoulder joint) can migrate upwards, causing it to rub against the acromion (part of the shoulder blade).
Common Symptoms of Shoulder Arthritis
Recognizing the symptoms of shoulder arthritis is the first step toward effective management. While symptoms can vary depending on the type and severity of arthritis, several common indicators suggest the presence of the condition.
Persistent Pain
Pain is a hallmark symptom of shoulder arthritis. Initially, the pain might be a dull ache, often described as a deep, throbbing sensation within the shoulder joint. This pain typically worsens with activity, particularly overhead movements or lifting objects. As the condition progresses, the pain can become more constant, even present at rest, and may interfere with sleep.
Stiffness and Decreased Range of Motion
Arthritis can cause the joint capsule to thicken and the cartilage to erode, leading to stiffness. Patients may notice a gradual loss of flexibility and range of motion in the affected shoulder. Simple tasks like reaching behind the back, combing hair, or putting on a coat can become increasingly difficult. This stiffness is often worse in the morning or after periods of inactivity.
Grinding, Popping, or Clicking Sensations (Crepitus)
As the smooth cartilage surfaces wear away, the bones within the joint can rub against each other. When the smooth surfaces are worn away, think of moving the shoulder around like driving on a cobblestone street. The friction of the bones rubbing may produce audible or palpable grinding, popping, clicking, or crunching sensations, known as crepitus, during shoulder movement.
Weakness
Patients may find it challenging to lift objects or perform activities that require shoulder strength. This weakness can further exacerbate functional limitations and impact daily living.
Swelling and Tenderness
Inflammation within the joint can lead to visible swelling and tenderness to the touch around the affected shoulder. This can be particularly common in inflammatory types of arthritis like rheumatoid arthritis, but may also occur in osteoarthritis.
Impact on Daily Activities and Sleep
The chronic nature of shoulder arthritis symptoms can significantly impact a patient’s quality of life. Everyday tasks, hobbies, and even professional responsibilities may become challenging or impossible. The persistent pain, especially at night, often disrupts sleep patterns, leading to fatigue, irritability, and a general decline in well-being.
Diagnosing Shoulder Arthritis
Accurate diagnosis is key to developing an effective treatment plan. The diagnostic process often begins with a detailed medical history, where your doctor will inquire about the onset, nature, and severity of pain, any previous injuries, family history of arthritis, and how symptoms affect daily activities. During the physical examination, your doctor may assess tenderness, range of motion, and strength.
Imaging may be utilized to support the diagnosis and assess the extent of joint damage. X-rays can reveal narrowing of the joint space, changes in bone shape, and bone spurs. For many cases of osteoarthritis, X-rays alone are sufficient for diagnosis. Magnetic resonance imaging (MRI) may be used in some cases to provide detailed images of soft tissues, including cartilage, tendons (like the rotator cuff), ligaments, and muscles. It is particularly useful for evaluating the extent of cartilage damage, identifying rotator cuff injuries that may coexist with arthritis, and detecting inflammation within the joint. CT scans can sometimes be utilized for surgical planning, but often are not needed to make the diagnosis.
Non-Surgical Treatment Options for Shoulder Arthritis
The initial approach to managing shoulder arthritis is typically conservative, focusing on alleviating pain, reducing inflammation, and preserving joint function without surgery. Non-surgical treatment options may include:
- Medications and Injections: Nonsteroidal anti-inflammatory drugs (NSAIDs) can help reduce pain and inflammation. Corticosteroid injections may be used to provide short-term relief from pain. Platelet-rich plasma (PRP) therapy, a regenerative treatment option, may be an option for some patients with mild arthritis.
- Physical Therapy: A tailored program can help maintain or improve joint mobility, strengthen the muscles surrounding the shoulder, and reduce pain. Initial exercises may focus on gentle range-of-motion to reduce stress on the joint, gradually progressing to resistance and strengthening exercises. Therapy is most effective in patients with mild arthritis, but for patients with bone-on-bone arthritis sometimes therapy can worsen the pain.
- Activity Modification: Adjusting daily activities to avoid movements that aggravate the shoulder can help reduce pain. This might involve modifying work tasks, changing exercise routines, or using assistive devices. Learning proper body mechanics and posture can also minimize stress on the joint.
Surgical Treatment Options
When non-surgical treatments no longer provide adequate pain relief or functional improvement, surgical intervention may be considered. The choice of surgical procedure can depend on the type and severity of arthritis, the patient’s age, activity level, and overall health.
Arthroscopy
Shoulder arthroscopy is a minimally invasive procedure where a small camera (arthroscope) and specialized instruments are inserted through tiny incisions. It may be used for less severe cases of arthritis to remove loose bodies, clean out inflamed tissue, and shave down bone spurs.
While minimally invasive surgery has become the standard for many procedures, ‘clean up’ arthroscopic surgeries for arthritis are less commonly offered as the results are less predictable. However, in the correct patient with more mild arthritis, it can still be a very good option.
Shoulder Replacement Surgery (Arthroplasty)
Shoulder replacement surgery, or arthroplasty, can be an effective treatment for severe shoulder arthritis, particularly when bone-on-bone friction is significant. The damaged parts of the shoulder joint are removed and replaced with artificial components (prostheses) made of metal and plastic. There are several types of shoulder replacement:
- Total (Anatomic) Shoulder Replacement: This procedure involves replacing both the humeral head (ball) and the glenoid (socket) components. This is typically performed for severe osteoarthritis when the rotator cuff is intact and functional.
- Reverse Shoulder Replacement: This innovative procedure was originally designed for patients with severe arthritis who also have an irreparable rotator cuff tear. In reverse shoulder replacement, the ball and socket components are reversed: a metal ball is fixed to the shoulder blade, and a plastic socket is attached to the upper arm bone. This design allows the deltoid muscle to power the arm, compensating for the damaged rotator cuff. More recently, the indications for reverse shoulder replacement have expanded, and it is now performed more commonly than anatomic shoulder replacements.
Preventing Shoulder Arthritis
While some risk factors for shoulder arthritis are beyond our control, several proactive measures may help reduce the risk of developing the condition or slow its progression:
- Regular, Low-Impact Exercise: Engaging in regular physical activity that strengthens the muscles around the shoulder without excessive impact can help improve joint stability and health. Examples include swimming, cycling, and walking.
- Proper Posture and Ergonomics: Maintaining good posture, especially during prolonged sitting or standing, helps distribute stress evenly across the shoulder joints. Using ergonomic setups at work can also reduce strain.
- Avoid Overuse and Repetitive Stress: If your activities or occupation involve repetitive overhead movements, take frequent breaks, vary your movements, and ensure proper technique to minimize stress on the shoulder.
- Protect Against Injuries: Take precautions to prevent shoulder injuries, such as wearing appropriate protective gear during sports, practicing safe lifting techniques, and avoiding falls.
- Warm-up and Stretch: Before engaging in physical activity, always perform a thorough warm-up to prepare muscles and joints. Incorporate stretching exercises to maintain flexibility and range of motion in the shoulder.
By adopting these preventive strategies, individuals can contribute to the long-term health of their shoulder joints.
Summary
Shoulder arthritis is a complex and often progressive condition that can significantly impact mobility and quality of life. Characterized by pain, stiffness, and reduced function, it encompasses various types, including osteoarthritis, rheumatoid arthritis, and post-traumatic arthritis, each with its unique pathology. Early recognition of symptoms, coupled with a thorough diagnostic process involving physical examination and imaging, is key to identifying the source of the pain and determining an effective treatment strategy.
A wide array of treatment options exists, beginning with conservative measures such as medication, physical therapy, and lifestyle modifications. When these approaches are insufficient, surgical interventions like arthroscopy or various forms of shoulder replacement may offer relief and functional restoration. While complete prevention may not always be possible, adopting healthy habits may help mitigate risk and slow disease progression.
Frequently Asked Questions
What are the symptoms of shoulder arthritis?
Common symptoms of shoulder arthritis include persistent pain, especially with activity or at night, and stiffness that makes everyday movements more difficult. Many patients also experience a decreased range of motion, making it hard to reach overhead or behind the back. Grinding, popping, or clicking sensations (called crepitus) may occur as cartilage wears down, and weakness may develop over time due to pain and reduced use. Some individuals also notice swelling or tenderness around the joint.
What is the difference between osteoarthritis and rheumatoid arthritis in the shoulder?
Osteoarthritisis a degenerative condition caused by the gradual wear and tear of joint cartilage, primarily affecting older individuals and often one shoulder. Rheumatoid arthritis, on the other hand, is an autoimmune disease where the body’s immune system attacks the joint lining, leading to inflammation and cartilage destruction.
Are there any specific exercises I should avoid if I have shoulder arthritis?
Generally, you may be advised to avoid exercises that cause sharp pain, excessive grinding, or clicking in your shoulder. High-impact activities, heavy lifting, and repetitive overhead movements that exacerbate symptoms should be limited or modified. A physical therapist can provide personalized guidance on safe and beneficial exercises, as well as those to avoid.
When should I see a doctor for shoulder pain?
Consider seeing a doctor if you experience persistent shoulder pain that does not improve with rest, if the pain interferes with your daily activities or sleep, if you notice significant stiffness or loss of motion, or if you have any grinding or popping sensations.



